Introduction: Delving into Alveolar Osteitis
When it comes to oral health complications, alveolar osteitis stands out as a condition that merits a closer examination. Often termed ‘dry socket,’ this dental dilemma surfaces following tooth extractions and can be a source of significant discomfort. But what propels alveolar osteitis into the spotlight of dental concerns, and why is it crucial to arm ourselves with knowledge about it?

In the journey of tooth recovery, the body typically follows a natural and uneventful healing process. However, alveolar osteitis disrupts this process, leading to exposed bone and a delayed healing timeline. It’s not just the pain that makes this condition noteworthy; it’s the complexity of factors that contribute to its onset and the multifaceted approach required for its treatment.
This condition doesn’t discriminate; it can affect anyone who has undergone dental extractions, although some are more susceptible than others. It’s a reminder of the delicate balance within our oral ecosystem and the importance of following post-operative care instructions to the letter.
With symptoms that can mimic other oral health issues, alveolar osteitis requires a discerning eye for proper diagnosis. Recognizing the signs early on is paramount, as timely intervention can dramatically ease the recovery process. It’s not merely about managing pain but also about preventing potential complications that can arise from an untreated condition.
As we delve deeper into the world of alveolar osteitis, we’ll uncover the layers of prevention, symptoms, and treatments. Understanding this condition is the first step in safeguarding our oral health and ensuring that our smiles remain as resilient as ever. Join us as we explore the critical aspects of alveolar osteitis, equipping you with the knowledge to face this dental challenge head-on.
1. The Onset of Alveolar Osteitis: A Closer Look at Initial Manifestations
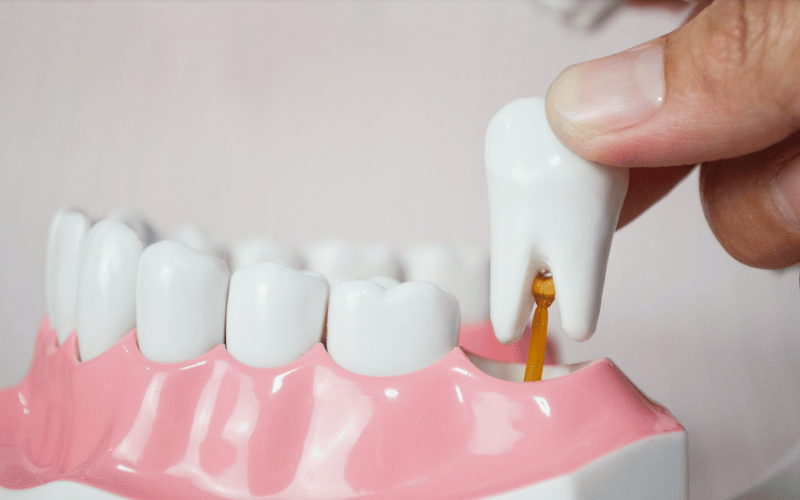
Alveolar osteitis typically rears its head a few days post-tooth extraction, a time when patients expect to be on the mend. The absence of a blood clot at the site of extraction, a cornerstone for healing, marks the beginning of this condition. Understanding the initial signs can mitigate the discomfort and prevent a prolonged recovery.
When the protective blood clot is dislodged or dissolves before the wound has healed, the underlying bone and nerves become exposed to the oral environment. This exposure is the primary culprit behind the intense pain associated with alveolar osteitis. It’s not a dull ache that one can ignore; the pain is sharp, persistent, and can radiate to the ear and neck.
Patients may also notice a distinct, unpleasant taste in their mouth, coupled with bad breath. These symptoms are often the body’s distress signals, indicating that all is not well within the extraction site. While pain is subjective, the severity in alveolar osteitis is such that it often prompts an immediate visit to the dentist.
The visual cues of alveolar osteitis are equally telling. Where one would expect to see a dark blood clot, there may instead be a visible bone or an empty-looking socket. This stark visual is sometimes the first indication for patients that their healing process is not progressing as it should.
Although alveolar osteitis is self-limiting, the discomfort it causes can be significant. Identifying these early signs is crucial in seeking timely dental interventions. These interventions can alleviate pain, protect the exposed area, and steer the recovery back on course. (1)