Introduction: The Importance of Early Detection

Rheumatoid arthritis (RA) is a perplexing condition with symptoms that are subtle yet serious. Often, the earliest symptoms mimic more innocuous health issues, leading to late diagnosis. Yet, an early diagnosis can dramatically improve management and prognosis, reducing the overall disease impact. To navigate this puzzle, we delve into the first ten symptoms of rheumatoid arthritis, highlighting their subtleties and significance.
Rheumatoid arthritis is no ordinary disease; it’s a medical conundrum. An autoimmune condition that primarily targets the joints, its emergence is silent, its progression slow, and its manifestations complex. Beneath the facade of normalcy, RA quietly chips away at the body’s defenses, silently preparing to launch a full-scale attack on the joints.
But while RA’s modus operandi may be subtle, it is not invincible. Like any complex puzzle, it too has tell-tale signs, patterns that betray its presence. These are the early symptoms of rheumatoid arthritis – silent, subtle, often overlooked, but unmistakable once you know what to look for.
At first glance, these symptoms seem commonplace – a little joint stiffness here, some tiredness there, perhaps a touch of fever. But when these pieces come together, they form a larger picture, revealing the lurking shadow of rheumatoid arthritis. Recognizing these early symptoms and their interconnections can help identify RA at its earliest stages, drastically improving the chances of managing the condition effectively.
Armed with this knowledge, the power to combat RA lies in your hands. The following sections will guide you through the ten early symptoms of rheumatoid arthritis, shedding light on each one’s unique characteristics and implications. By understanding these signs, you can transform vague worries into concrete actions, arming yourself with the tools to tackle this invisible enemy head-on.
Symptom 1. Joint Pain: The Classic Sign of Rheumatoid Arthritis
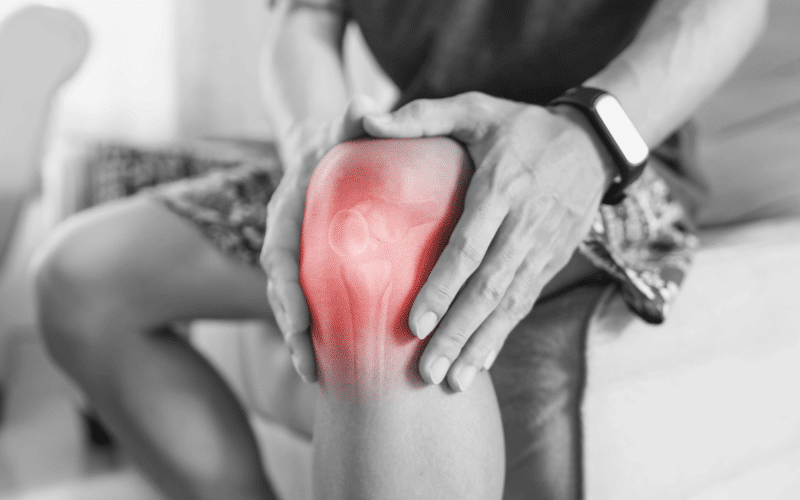
Joint pain is the quintessential harbinger of rheumatoid arthritis. As the disease sets in, it launches a silent assault on the synovial joints. This assault triggers a chain reaction of inflammation and discomfort, leading to the characteristic pain associated with RA.
In rheumatoid arthritis, joint pain is more than just a casual inconvenience. It’s a persistent ache that gnaws at the joints, often starting in the hands and feet before spreading to larger joints. What sets this pain apart is its bilateral nature; it tends to affect the same joints on both sides of the body.
The pain associated with RA is peculiar. It’s not a sharp, stabbing sensation but more of a dull, constant ache. This sensation is especially noticeable during periods of rest or upon waking up in the morning. The pain can also worsen during periods of activity, adding another layer of complexity to this symptom.
RA-related joint pain is not limited to a specific joint or region. Instead, it jumps from one joint to another, causing a condition known as migratory arthritis. This pattern can create a trail of pain that moves across various joints over time.
Lastly, it’s essential to remember that RA-related joint pain is not static. It can fluctuate in intensity and duration, with periods of increased disease activity known as ‘flares’. During these flares, joint pain can escalate, further confirming the underlying presence of rheumatoid arthritis. (1)