Introduction: An In-Depth Look at Thyroidectomy Surgery
Thyroidectomy surgery marks a turning point for those grappling with thyroid disorders. This detailed, multi-step operation is often the definitive solution to a range of thyroid-related ailments that impede everyday life. Our goal is to elucidate the intricate process and demystify the experience for patients about to embark on this journey.
The thyroid, a butterfly-shaped gland at the base of the neck, has an outsized impact on bodily function, despite its small size. It produces hormones that regulate metabolism, meaning its performance is integral to a person’s overall well-being. The most common conditions necessitating thyroidectomy include hyperthyroidism, hypothyroidism, and nodular thyroid disease. Each presents unique challenges, with symptoms that can range from inconvenient to life-threatening.
So, what does it mean to undergo a thyroidectomy? This operation involves the surgical removal of either part or all of the thyroid gland. Such a drastic solution is not the first resort; typically, it is considered when other treatment methods fail to bring about relief or when the presence of nodules raises the specter of cancer.
The decision to proceed with a thyroidectomy, like any significant medical procedure, involves careful deliberation and planning. Patients must receive comprehensive information about what to expect before, during, and after the operation. In the following sections, we will break down these stages into 15 digestible steps, offering clear, insightful descriptions of each phase.
Step 1: The Doorway to Diagnosis: Confirming the Need for Thyroidectomy
At the heart of every successful thyroidectomy lies a comprehensive diagnosis process. It’s akin to unlocking a door, behind which the reality of the patient’s health condition hides.
The initial consultation is the first key to this door. This is when doctors conduct a thorough evaluation of the patient’s symptoms. Persistent fatigue, difficulty sleeping, weight fluctuations, and mood swings are a few signs pointing towards potential thyroid dysfunction. This process, layered with details, aims to paint a comprehensive picture of the patient’s health condition.
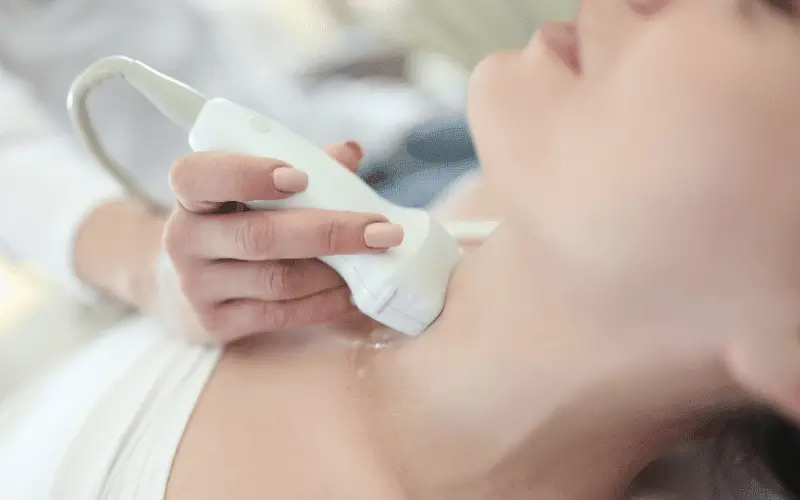
The second key comes in the form of diagnostic tests. Comprehensive blood work and imaging scans such as ultrasounds or radioactive iodine scans are commonly employed. They don’t just examine the thyroid gland’s physical condition but also assess hormone levels, pointing towards hyperthyroidism or hypothyroidism. This step demystifies the patient’s experience, transforming abstract symptoms into concrete data.
Analyzing these results, doctors can identify patterns and irregularities. Is the thyroid producing an excessive amount of hormones, leading to hyperthyroidism? Or is it underactive, causing hypothyroidism? Alternatively, are there physical abnormalities like nodules or goiters present? This third key turns the lock, providing clarity about the health issue at hand.
Based on the diagnosis, if a thyroidectomy is deemed the optimal solution, the patient is informed. It’s a indispensable conversation, revealing the reality behind the door. The patient is educated about the procedure, the reason behind this choice, and what it means for their life post-surgery. This information is paramount to making an informed decision.
Lastly, a personalized treatment plan is charted out. It’s like a roadmap, delineating the course the patient will follow – a course that leads to recovery. Each patient’s journey is unique, and their treatment plan reflects this individuality. It’s this intricate dance of diagnostics and decision-making that heralds the beginning of the thyroidectomy journey. (1)