Introduction: The Battle of the Thyroids: Papillary vs. Follicular
Unraveling the mysteries of the human body often leads us down paths rife with complexity and nuance. When discussing thyroid cancer, the two primary culprits we encounter are Papillary Thyroid Cancer (PTC) and Follicular Thyroid Cancer (FTC). They stand as the most common varieties of this disease, each affecting the lives of millions worldwide.
Though PTC and FTC share numerous similarities, they are far from identical. The disparities that exist between them manifest in a variety of areas, including their prevalence, risk factors, pathological attributes, treatment methods, and prognoses.
The importance of discerning these differences cannot be understated. It is through such comprehension that we can better understand these cancers, thereby improving strategies for diagnosis, treatment, and patient outcomes.
This exploration is not merely academic—it carries significant implications for patients, healthcare professionals, and those affected by thyroid cancer. By equipping ourselves with detailed knowledge about PTC and FTC, we gain the power to approach this disease more effectively, optimally influencing clinical practices and patient care.
In today’s discussion, we will delve deep into the world of thyroid cancers, investigating the distinct aspects of PTC and FTC. Join us as we dissect the complexities and unique characteristics of these diseases.
1. Prevalence: Papillary vs. Follicular Thyroid Cancer – A Tale of Two Incidences
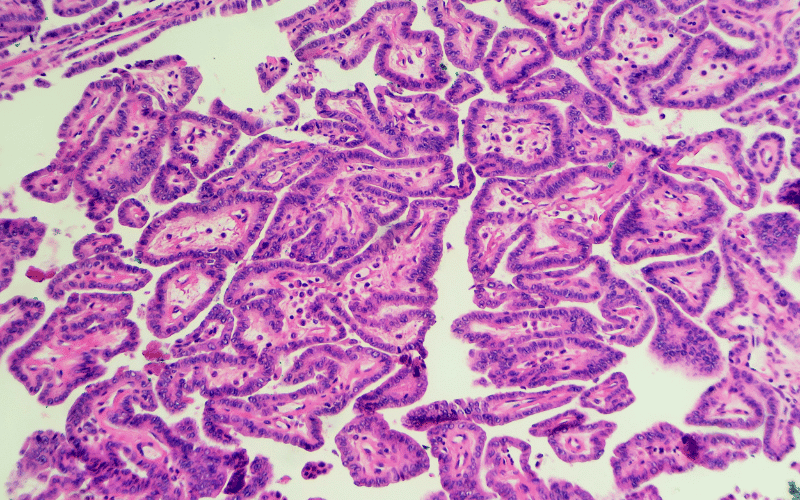
The onset of our journey takes us to the epidemiological landscape of Papillary Thyroid Cancer (PTC) and Follicular Thyroid Cancer (FTC). This first step is crucial because it sets the scene, providing a broader understanding of how common these cancers are in different population groups.
To begin with, PTC takes the lead as the most common type of thyroid cancer. It accounts for about 85% of all thyroid cancer cases.
An interesting point to note here is the predilection of PTC for younger patients, often diagnosed in the 30 to 50 age bracket. Furthermore, it has a significantly higher incidence rate in women compared to men, with women being three times more likely to develop PTC.
On the other hand, FTC, although less common, is still a significant player in the field of thyroid cancers. FTC constitutes approximately 10% to 15% of all thyroid cancer cases.
It typically affects an older demographic than PTC, usually occurring in people aged 50 or older. Similar to PTC, FTC shows a higher occurrence rate in women. However, the gender disparity is less marked in FTC when compared to PTC.
Now, an intriguing question arises here – why are these cancers more prevalent in women and in certain age groups? It appears that hormonal influences, particularly those relating to estrogen, may play a key role.
This theory is supported by the observation that the gender disparity in incidence rates becomes less pronounced after women reach menopause. Undoubtedly, there is much more to uncover about the influence of hormones on thyroid cancer development, and ongoing research continues to shed light on this complex interplay.
PTC and FTC exhibit marked differences in their prevalence rates, affected age groups, and gender predilection. These aspects contribute significantly to our understanding of the disease epidemiology and influence the strategies employed for early detection and prevention. (1)