Introduction: Delving into Mycosis Fungoides
When considering skin ailments, it’s easy to overlook some of the rarer conditions that don’t garner as much attention. Amidst the more common skin problems, mycosis fungoides, also known as granuloma fungoides or Alibert Bazin syndrome, stands out. Just as you’d approach the top mortgage companies for a housing loan, it’s equally important to address unusual skin symptoms with the same urgency. This article aims to shed light on this often-overlooked skin condition.
Delving into the world of skin disorders often reveals a myriad of conditions ranging from the benign to the severe. Mycosis fungoides, despite its rarity, demands attention due to the severe implications it can have on those affected. Much like navigating the housing market, understanding the early signs and symptoms can save you a great deal of trouble down the line.
Skin disorders come in various forms, and many are commonly known. Conditions like eczema or psoriasis are frequently discussed and have become household names.
Yet, there’s a spectrum of skin diseases, many of which don’t get the limelight they deserve. Mycosis fungoides, for instance, is a rare type of cutaneous T-cell lymphoma.
While its name may sound exotic, the effects it has on its sufferers are profound. The condition primarily affects the skin but originates in the white blood cells.
Early diagnosis is always a boon in medical scenarios. Much like securing a mortgage from a trusted company ensures a smooth home-buying process, identifying symptoms of mycosis fungoides at an early stage can greatly impact health outcomes. Hence, it’s vital to be equipped with the knowledge to spot these signs.
1. Patches on the Skin: The Silent Prelude to Mycosis Fungoides
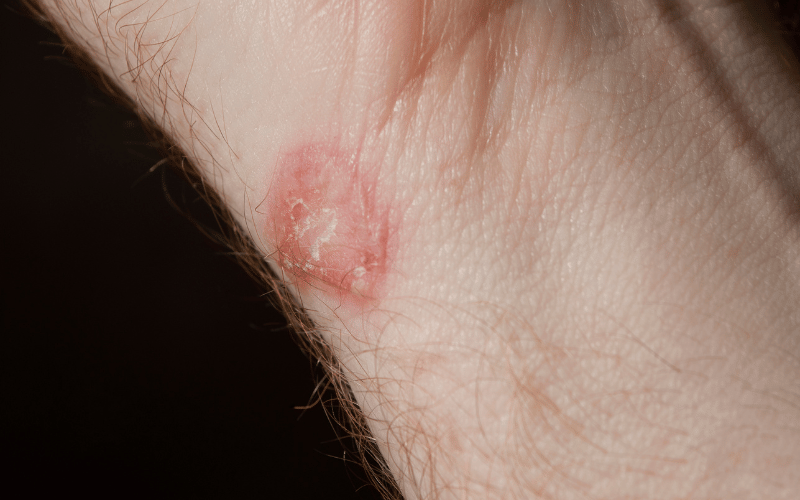
One of the earliest indications of mycosis fungoides is the appearance of patches on the skin. Often inconspicuous at first, these thin, reddened patches may seem like a mere rash or a fleeting skin irritation.
They don’t bring with them the alarm that other symptoms might later on. On closer observation, they are usually flat, reddish, and possess a slightly scaly texture. These patches, while often overlooked, are crucial in the early detection of mycosis fungoides.
The reason behind these patches is the accumulation of malignant T-cells in the skin. As these abnormal cells begin to cluster, they cause discoloration, leading to these patches.
It’s intriguing how our body signals an internal issue through such external signs. However, the real challenge is differentiating these patches from other common skin conditions, such as eczema or dermatitis. The patches in mycosis fungoides are chronic and do not tend to resolve on their own, which is one of their distinguishing characteristics.
Location is another telltale sign. These patches, in the early stages of mycosis fungoides, have a predilection for certain areas of the body. They are most commonly found on the buttocks, hips, and the sides of the torso.
It’s not uncommon for patients to dismiss them as mere skin irritations, especially if they aren’t causing any discomfort. However, a distinguishing factor is their persistence. Unlike a rash from an allergic reaction that might disappear in a few days or weeks, these patches linger and may even expand over time.
Identifying these patches in their early stage can significantly influence the disease’s trajectory. Since mycosis fungoides is a progressive condition, early intervention can curb its advancement.
The patches themselves, while not overly bothersome, serve as a clarion call to seek medical advice. While they might not be itchy or painful in every individual, their presence is a manifestation of an underlying issue that needs addressing. Catching the disease at this phase allows for a broader range of treatment options and can significantly impact the overall prognosis. (1)